You may think of measles as a childhood illness marked by fever and a rash. For many, it’s seen as something uncomfortable but temporary. But science is showing a far more serious reality—one that extends beyond the initial infection and into the brain itself.
Recent research has revealed that measles doesn’t always end when the rash fades. In some cases, the virus can remain hidden in the body and later trigger devastating neurological conditions. These complications can develop years after the initial infection, often when families least expect it.
What Happens When Measles Infects the Body
Measles is caused by a highly contagious virus that spreads through respiratory droplets. Once it enters your body, it doesn’t just stay in the lungs or throat. It travels through your bloodstream and can affect multiple systems.
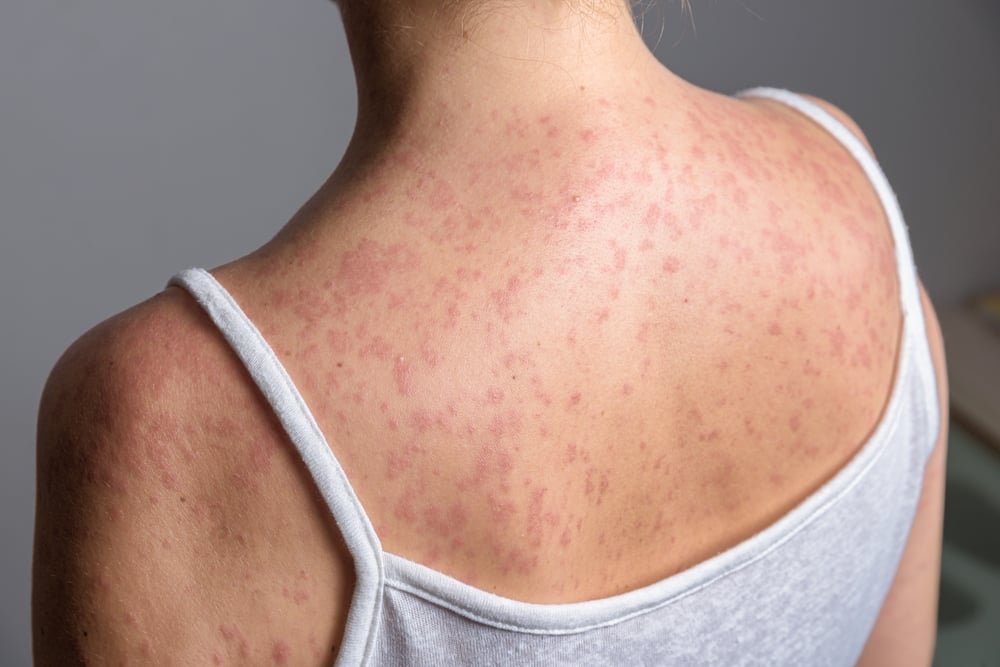
Initially, symptoms include fever, cough, runny nose, and inflamed eyes, followed by the classic rash. During this phase, your immune system works hard to fight off the infection. Most people recover within a few weeks.
However, measles has a unique ability that sets it apart from many other viruses. It can suppress your immune system. This phenomenon, sometimes referred to as “immune amnesia,” weakens your body’s ability to remember and fight off other infections for months or even years.
This alone is concerning. But for some individuals, the virus takes a far more dangerous path.
The Brain Complications You Don’t See Coming
In rare but serious cases, measles can lead to neurological complications. These range from acute conditions to delayed, progressive diseases that appear years later.
Acute Encephalitis
Shortly after infection, some individuals develop encephalitis, which is inflammation of the brain. This can cause seizures, confusion, and even permanent brain damage. According to the Centers for Disease Control and Prevention (CDC), about 1 in 1,000 measles cases leads to this complication.
Subacute Sclerosing Panencephalitis (SSPE)
One of the most alarming consequences of measles is a condition called subacute sclerosing panencephalitis, or SSPE.
This is a rare but fatal brain disorder that develops years after a person seems to have recovered from measles. The virus remains in the brain in a mutated form, slowly damaging brain tissue over time.
Symptoms often begin subtly, with personality changes or memory issues. Over time, they progress to seizures, loss of motor control, and severe cognitive decline. Eventually, the disease leads to death.
Children who contract measles at a very young age are at a higher risk of developing SSPE later in life.
How Measles “Hides” in the Brain
What makes SSPE particularly frightening is how the virus behaves. Instead of being fully cleared from the body, it can persist in brain cells.
Scientists believe that the measles virus undergoes mutations that allow it to evade the immune system. These altered viral particles don’t spread in the usual way but instead move slowly from neuron to neuron.
Over time, this leads to widespread inflammation and destruction of brain tissue.
Research using advanced imaging and molecular techniques has helped scientists better understand how this process unfolds. They’ve observed structural damage in brain regions responsible for movement, memory, and cognition, explaining the severe symptoms seen in SSPE patients.
Why Children Are Especially Vulnerable
Young children face the greatest risk when it comes to severe measles complications.
Their immune systems are still developing, which makes it harder for their bodies to fully eliminate the virus. This increases the likelihood that the virus may persist in a latent form.
Studies have shown that children infected with measles before the age of two are significantly more likely to develop SSPE compared to those infected later in life.
This is one of the reasons why measles is not just a mild childhood illness. Timing matters, and early exposure can have lifelong consequences.
The Role of Vaccination in Prevention
The good news is that measles is preventable. Vaccination remains the most effective way to protect yourself and your family from both the immediate and long-term dangers of the virus.
The measles, mumps, and rubella (MMR) vaccine has been shown to be highly effective. It not only prevents infection but also eliminates the risk of complications like SSPE.
When vaccination rates drop, outbreaks can occur. This increases the risk for vulnerable populations, including infants who are too young to be vaccinated and individuals with weakened immune systems.
From a public health perspective, maintaining high vaccination coverage helps protect entire communities.
What This Means for Your Brain Health
When you think about brain health, you might focus on diet, sleep, or stress management. But infections play a role that is often overlooked.
Viruses like measles can have lasting effects on the brain, even long after the initial illness seems to have passed. This is why prevention is not just about avoiding a temporary sickness. It’s about protecting your long-term neurological function.
Your brain is one of your most valuable organs. Safeguarding it requires a proactive approach that includes vaccination, immune support, and awareness of potential risks.
My Personal RX on Protecting Your Brain From Hidden Viral Threats
Protecting your brain starts with understanding that not all damage is immediate. Some threats develop quietly over time, and your daily choices can make a meaningful difference. Here are my personal recommendations to help you stay ahead of these risks:
1. Stay Up to Date on Vaccinations: Ensure that you and your family are current with recommended vaccines, including the MMR vaccine. Prevention is your first and most effective defense.
2. Support Your Immune System Daily: A strong immune system helps your body respond effectively to infections. Focus on whole foods rich in vitamins A, C, and D, along with zinc and antioxidants.
3. Prioritize Gut Health: Your gut and brain are closely connected. Supporting your microbiome with a high-quality probiotic like MindBiotic can help regulate immune responses and inflammation.
4. Eat Brain-Boosting Foods: Incorporate foods rich in omega-3 fatty acids, such as salmon, walnuts, and flaxseeds. These nutrients support cognitive function and reduce inflammation.
5. Get Consistent, Restorative Sleep: Sleep is when your brain clears toxins and repairs itself. Aim for 7–9 hours of quality sleep each night to support neurological health.
6. Manage Inflammation: Chronic inflammation can worsen the effects of infections. Add anti-inflammatory foods like turmeric, leafy greens, and berries to your diet.
7. Reduce Exposure to Illness: Practice good hygiene, especially during outbreaks. Regular handwashing and avoiding close contact with sick individuals can reduce your risk.
8. Stay Informed, Not Fearful: Understanding the risks allows you to take action. Educate yourself from reliable sources so you can make confident health decisions.
9. Incorporate Targeted Supplements: Consider adding high-quality supplements that support both brain and immune health. Products designed to enhance cognitive clarity and resilience can be beneficial.
10. Feed Your Mind With Knowledge: My book, Heal Your Gut, Save Your Brain, explains how your digestive health influences your brain. Learning this connection can help you take better control of your overall well-being.
Source:
- Kung, M. S., & Crawford, J. R. (2026). Subacute Sclerosing Panencephalitis after Measles Infection. New England Journal of Medicine, 394(9), e14. https://doi.org/10.1056/nejmicm2504828










 Subscribe to Ask Dr. Nandi YouTube Channel
Subscribe to Ask Dr. Nandi YouTube Channel










