Every year, 100,000 Americans die of blood clots — and shockingly, 1 out of 4 get no warning before it happens. [1]
Your body’s circulatory system is a complex network that carries life-sustaining essentials. Blood clotting is one of its essential processes, which stops bleeding when you’re injured. But what happens when this process goes awry, leading to blood clots where they shouldn’t be?
Blood clotting is a fundamental process that aids in healing wounds. However, the formation of blood clots within veins without an associated injury can indicate a severe health concern. Recognizing the initial signs of these internal blood clots is imperative for timely treatment and prevention of potentially life-threatening conditions.
What Is Blood Clot and How Does It Form?
Blood clotting, a remarkable physiological process, emerges as a safeguard mechanism when the body encounters injury. Platelets, small cell fragments in the blood, and proteins called clotting factors orchestrate this phenomenon.
When a blood vessel is injured, platelets rush to the site, forming a temporary plug to prevent excessive bleeding. Simultaneously, clotting factors activate a cascade of reactions, eventually leading to the conversion of fibrinogen, a soluble protein, into fibrin, an insoluble fiber-like substance. This fibrin mesh reinforces the platelet plug, creating a robust clot that staunches the wound and promotes healing. [2,3]
However, this process can occasionally misfire, leading to internal blood clots in veins without apparent injury. Factors such as prolonged immobility, certain medical conditions, or genetic predisposition can contribute to this aberrant clotting. When this happens, the consequences can be dire, potentially causing conditions like deep vein thrombosis (DVT) and pulmonary embolism (PE).
Unraveling the Causes: Risk Factors and Conditions
Blood clots can form without apparent reasons due to a variety of risk factors and conditions. Scientific studies have shown that the following factors can contribute to their formation:
- Prolonged periods of sitting, such as during work or travel
- Extended bed rest due to illness, hospitalization, or surgical procedures
- Pregnancy, certain hormonal medications, smoking, or obesity
- Certain types of cancer, including pancreatic, lung, multiple myeloma, or blood-related cancers
- A family history of blood clots
- Chronic inflammatory diseases
- Certain infections, such as HIV/AIDS, hepatitis C, or Lyme disease
- Autoimmune disorders
Research has indicated the interplay between these factors and the body’s clotting mechanisms, shedding light on why clots might form even in the absence of apparent injury or trauma.

The Two Sides of Blood Clots: Arterial and Venous
Blood clots can manifest in both arteries and veins, each with its own set of implications. Arterial clots, often associated with arteriosclerosis, can lead to heart attacks or strokes, causing profound damage to vital organs.
On the other hand, venous clots, like deep vein thrombosis (DVT), can obstruct blood flow, resulting in pain and swelling. The most severe form of venous blood clot can lead to pulmonary embolism (PE) when a clot detaches and travels to the lungs, posing life-threatening consequences. [4]
Identifying the Culprits: 6 Warning Signs of Blood Clots
Recognizing the symptoms of blood clots can be a matter of life and death. Research has outlined six key warning signs that require your attention:
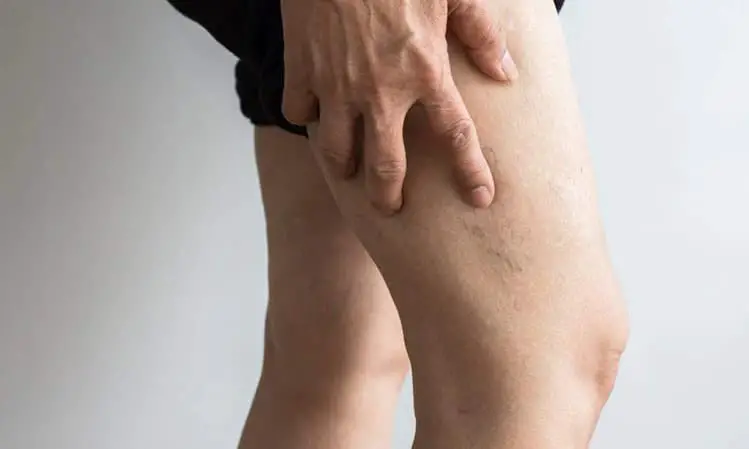
1. Sudden Swelling: A clot in the lower leg can cause sudden swelling in one ankle or shin, accompanied by pain, tenderness, warmth, and a reddish discoloration at the site.
2. Racing Heart: Rapid heartbeat may indicate a blood clot in the lungs as the heart attempts to compensate for restricted blood flow.
3. Chest Pain: Sharp chest pain, especially while breathing deeply, could signal a pulmonary embolism. This pain may also occur during coughing, bending, or stooping.
4. Unexplained Cough: A sudden dry cough, particularly if it produces bloody or blood-streaked sputum, could be indicative of a blood clot.
5. Vomiting: Severe abdominal pain, accompanied by nausea and vomiting, might suggest a blood clot in the abdomen. Additional symptoms could include fever or an urgent need for bowel movement.
6. Impaired Vision: Sudden blurry or complete loss of vision in one eye might result from a clot in the vessel carrying blood to the eye’s retina. Central retinal artery occlusion (CRAO) can lead to such visual disturbances.
Treatments for Blood Clots
Managing the onset of blood clots is pivotal for maintaining cardiovascular health and preventing life-threatening complications. The approach, however, varies based on the type of clot, its location, and individual risk factors. Here’s a look at some common treatments and preventative measures:
- Anticoagulants: Often referred to as blood thinners, these medications don’t actually thin the blood but rather prevent it from clotting as easily. Examples include warfarin (Coumadin, Jantoven) and heparin. Newer oral anticoagulants such as rivaroxaban (Xarelto) and apixaban (Eliquis) are also becoming increasingly popular.
- Thrombolytics: These are clot-dissolving drugs used to treat certain types of clots like those seen in pulmonary embolism or stroke. They work quickly but carry the risk of serious bleeding, so they’re reserved for life-threatening situations.
- Compression stockings: These special stockings apply pressure to your lower legs, helping to reduce pain and swelling and prevent clots from forming.
- Surgery or catheter-directed thrombolysis: In severe cases, especially when the clot is large, doctors may use surgical or minimally invasive techniques to remove a clot. [5,6]

My Personal RX: Preventing and Managing Blood Clots
Prevention is a cornerstone of maintaining optimal health. Scientific research has established that managing certain risk factors can significantly reduce the likelihood of blood clot development. Here are some key measures to consider:
- Lifestyle Changes: Adopting a healthier lifestyle is the foundation for blood clot prevention. This includes regular exercise, a balanced diet, avoiding smoking, and managing conditions like diabetes and high blood pressure.
- Regular Movement: If you’re on a long flight or drive, make sure to stand up, stretch, and walk around every 1-2 hours. If hospitalized or bedridden, rotating your ankles and wiggling your toes can help.
- Stay Hydrated: Drinking plenty of water can prevent dehydration, which could increase the risk of clot formation.
- Empower Your Well-Being: Access a free copy of my comprehensive 50-page Protocol for Optimizing Your Health and Wellbeing Protocol. This resource holds the key to fostering profound, enduring transformations in your life and health.
- Support Your Body: Elevating glutathione levels supports respiratory, hepatic, and immune health while offering antioxidant protection against inflammation. With the added benefit of reducing mucus viscosity, pure NAC also promotes respiratory and pulmonary vitality. Give your body the support it needs with Pure N-Acetyl Cysteine (NAC).
- Regular Check-ups: Regular visits to a healthcare professional can help assess your risk factors and guide you in taking the necessary preventative measures.
While preventive measures are essential, awareness of the signs and risks associated with blood clots can be life-saving. Remember, you are the best advocate for your own health. If something doesn’t feel right, don’t hesitate to consult a medical professional promptly.

Sources:
- Impact of blood clots on the United States | CDC. (2018, October 19). Centers for Disease Control and Prevention. https://www.cdc.gov/ncbddd/dvt/infographic-impact.html
- Blood clots. (n.d.). Hematology.org. https://www.hematology.org/education/patients/blood-clots
- Garmo, C. (2022, September 5). Physiology, clotting mechanism. StatPearls – NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK507795/
- Prandoni, P. (2009b). Venous and arterial thrombosis: Two aspects of the same disease? Clinical Epidemiology, 1. https://doi.org/10.2147/clep.s4780
- Blood clot treatment. (n.d.). Johns Hopkins Medicine. https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/blood-clot-treatment
- National Blood Clot Alliance. (2023, July 14). Blood clot treatment – Blood clots. Blood Clots. https://www.stoptheclot.org/about-clots/blood-clot-treatment/









 Subscribe to Ask Dr. Nandi YouTube Channel
Subscribe to Ask Dr. Nandi YouTube Channel










