For decades, doctors have told osteoarthritis patients the same thing: manage the pain, lose some weight, and accept that the damage is done. No drug on the market can rebuild worn-down cartilage or reverse the breakdown happening inside your joints. Treatment has been about coping, not curing. But a new study just changed that conversation. Researchers discovered that semaglutide, the drug behind Ozempic and Wegovy, appears to repair joint cartilage in both mice and humans through a mechanism nobody expected. It has nothing to do with losing weight. Something else is happening at the cellular level, and it could reshape how medicine treats the most common form of arthritis on the planet.
Osteoarthritis: A Disease With No Real Fix
Osteoarthritis affects roughly 600 million people worldwide. By 2050, that number is expected to reach one billion. It is the most common form of arthritis and a leading cause of disability, especially among older adults. But it is also rising among younger, active populations, leaving people in their 30s and 40s facing decades of joint pain and limited mobility.
Inside an osteoarthritic joint, cartilage breaks down over time. Cartilage is the smooth, rubbery tissue that cushions the ends of bones where they meet. When it wears away, bones grind against each other, causing pain, swelling, stiffness, and eventual loss of movement. Bone spurs can form. Joint membranes become inflamed. Eventually, the entire joint fails.
Current treatments are palliative. Pain medications, physical therapy, steroid injections, and hyaluronic acid shots can ease symptoms, but none of them stop or reverse the underlying destruction. Joint replacement surgery is the last resort when everything else fails.
Obesity, diabetes, high cholesterol, and chronic inflammation all accelerate osteoarthritis progression. These metabolic conditions damage cartilage, bone, and the synovial membrane that lubricates joint surfaces. A distinct subtype called “metabolic osteoarthritis” has emerged in medical literature, recognizing that joint breakdown often starts with metabolic dysfunction, not just mechanical wear.

Semaglutide: A Drug Built for Something Else Entirely
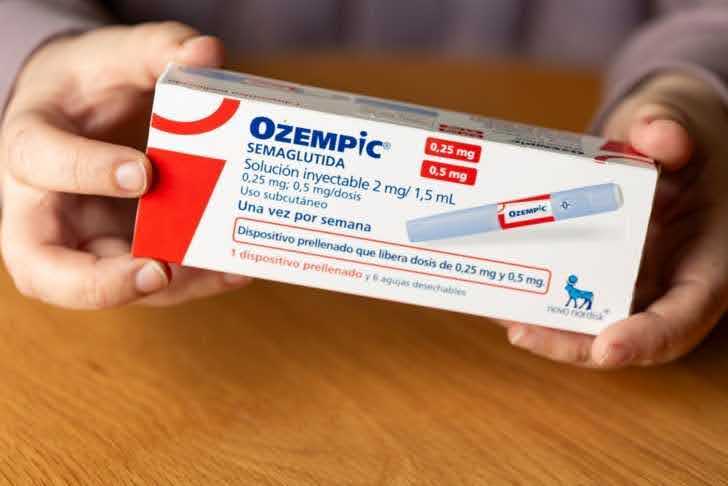
Semaglutide is a GLP-1 receptor agonist. It mimics a natural hormone called glucagon-like peptide 1 (GLP-1), which stimulates insulin release, manages blood sugar, and tells your brain that you are full. Drugs built on semaglutide, like Ozempic (for type 2 diabetes) and Wegovy (for weight loss), have become some of the most prescribed medications in the world.
Given the strong link between obesity and osteoarthritis, it seemed obvious that semaglutide might help joints by helping people lose weight. Less body weight means less mechanical load on knees, hips, and ankles. Case closed.
The researchers behind this new study, published in Cell Metabolism, proved that weight loss is not the explanation. Something far more interesting is going on inside the cartilage itself.
A Clever Control Group Cracked the Case
A team from Shenzhen Institutes of Advanced Technology (Chinese Academy of Sciences), Washington University School of Medicine, and the University of Aberdeen designed an experiment to isolate semaglutide’s effect on joints from its effect on appetite and weight.
They created obese mice with surgically induced osteoarthritis and split them into groups. One group received semaglutide. Another group, called the “pair-feeding” group, ate the same amount of food as the semaglutide-treated mice. Both groups lost similar amounts of weight.
Here is where the results split. Semaglutide-treated mice showed significant cartilage protection. Their joints had less cartilage breakdown, fewer bone spurs, less joint membrane damage, and reduced pain sensitivity. Mice in the pair-feeding group, despite identical weight loss, received none of those benefits. Their joints deteriorated like those of untreated mice.
That single finding changes the entire story. Semaglutide is not protecting joints because of weight loss. It is doing something directly to the cells inside the cartilage.
Reprogramming How Cartilage Cells Produce Energy
To find out what semaglutide was doing at the cellular level, researchers compared cartilage from treated and untreated mice. They detected changes in the expression of nearly 8,300 proteins. Among the most affected pathways were those related to metabolism, specifically how cartilage cells (called chondrocytes) produce energy.
In healthy cartilage, chondrocytes get most of their energy through a process called glycolysis. Glycolysis works fast and does not need oxygen, but it is inefficient. It produces only two molecules of ATP (the cell’s energy currency) per molecule of glucose.
In osteoarthritic joints, glycolysis becomes even more dominant as cells scramble to meet rising energy demands for repair and survival. But the energy output is simply not enough. Cells burn through glucose fast, produce excessive lactate as a byproduct, and still run out of fuel. When ATP drops too low, chondrocytes stop functioning, stop repairing cartilage, and eventually die.
Semaglutide flipped that equation. After treatment, chondrocytes shifted their primary energy source from glycolysis to oxidative phosphorylation (OXPHOS). OXPHOS uses oxygen and is far more efficient, producing up to 36 ATP molecules per glucose molecule. With more ATP available, chondrocytes could repair damaged cartilage, produce collagen, and survive under inflammatory stress.
In normal chondrocytes, OXPHOS accounted for about 54% of energy production. Under osteoarthritic conditions, glycolysis dominated at nearly 87%. After semaglutide treatment, the balance was restored to roughly equal contributions from both pathways, giving cells enough energy to both function and heal.
The Molecular Pathway: GLP-1R to AMPK to PFKFB3
Researchers traced the full signaling chain behind semaglutide’s effect. When semaglutide binds to GLP-1 receptors on chondrocytes, it triggers a cascade of enzymes. First, it activates PKA (protein kinase A), which then activates AMPK (a master sensor of cellular energy). AMPK, in turn, switches on PFKFB3, a rate-limiting enzyme that regulates glycolytic flux and links it to mitochondrial metabolism.
Researchers called this the “GLP-1R-AMPK-PFKFB3 axis.” To confirm it was essential, they created genetically modified mice. When they knocked out the GLP-1 receptor gene, semaglutide’s protective effects disappeared completely. The drug could not reduce cartilage damage, bone spurs, or pain without the receptor present.
When they knocked out the AMPK gene specifically in cartilage cells, semaglutide’s benefits were similarly abolished. No cartilage protection. No pain relief. AMPK was confirmed as a non-negotiable link in the chain.
It Worked in Humans Too
Mouse studies are one thing. Human results are another. So the team ran a small randomized pilot clinical study to test whether semaglutide’s cartilage-protective effects would translate to real patients.
They enrolled 20 people aged 50 to 75, all with both obesity and knee osteoarthritis. Half received hyaluronic acid injections alone (a standard joint-lubricating treatment). Half received hyaluronic acid plus semaglutide.
After 24 weeks, the group receiving both treatments showed greater improvement in knee function scores compared to the hyaluronic acid-only group. MRI scans revealed something even more striking: cartilage in the combination group grew thicker by about 17%. Enhanced clarity at the cartilage-subchondral bone interface suggested new cartilage formation was occurring. In the hyaluronic acid-only group, cartilage thickness changed by less than 1%. In a disease where no approved drug rebuilds cartilage, a 17% increase in cartilage thickness after just 24 weeks is a remarkable result.

Why Caution Still Matters
Despite the exciting findings, the researchers urged restraint. The human trial was small (only 20 participants), and the MRI resolution used has limitations for measuring cartilage at sub-millimeter levels. Semaglutide also comes with known side effects, including nausea, gastrointestinal discomfort, and other concerns that may affect long-term use.
Mouse studies do not always predict human outcomes, and long-term cartilage regeneration has not yet been confirmed in larger populations. Much bigger, well-powered clinical trials are needed before semaglutide could be recommended or approved specifically for osteoarthritis treatment.
As the researchers wrote, the protective effects of semaglutide on the human knee joint should be interpreted with caution and require further validation by clinical trials.
What This Means for the Future of Joint Health
Even with those caveats, the implications are significant. For the first time, a drug has shown the ability to reverse cartilage damage through a metabolic mechanism that does not depend on weight loss. If larger trials confirm these findings, semaglutide or similar GLP-1 drugs could become the first disease-modifying treatments for osteoarthritis, shifting the field from symptom management to actual repair.
With osteoarthritis projected to affect one billion people within 25 years, and with the disease increasingly hitting younger populations, the need for effective treatments has never been greater. A drug that reprograms how cartilage cells produce energy and helps them rebuild damaged tissue could change millions of lives.
My Personal RX on Protecting Your Joints and Fighting Osteoarthritis
Osteoarthritis does not appear overnight. It builds over the years through inflammation, metabolic stress, and wear on joint cartilage. While we wait for drugs like semaglutide to be studied further for joint repair, you can take daily steps to protect your cartilage, reduce inflammation, and support joint health starting now. I always tell my patients that healthy joints depend on what you eat, how you move, how you sleep, and how well your body controls inflammation. Here is what I recommend:
- Prioritize Deep, Restorative Sleep: Your body repairs cartilage and other tissues during deep sleep. Sleep Max combines magnesium, GABA, 5-HTP, and taurine to calm your mind, support neurotransmitter balance, and promote restorative REM sleep so your joints and tissues can recover each night.
- Know Your Supplement Gaps: After 40, your body absorbs fewer key nutrients needed for joint and bone health. Download my free guide, The 7 Supplements You Can’t Live Without, to learn which supplements matter most, which “healthy” foods may be misleading you, and how to spot quality products.
- Move Daily, But Move Smart: Low-impact exercise like walking, swimming, and cycling strengthens the muscles around your joints without adding excessive stress. Aim for at least 30 minutes of movement most days to keep joints lubricated and flexible.
- Maintain a Healthy Weight: Excess body weight places direct mechanical stress on weight-bearing joints and increases systemic inflammation. Even modest weight loss of 5% to 10% of body weight can significantly reduce knee pain and slow cartilage loss.
- Add Collagen-Supporting Foods to Your Diet: Bone broth, fish with skin, citrus fruits, bell peppers, and leafy greens provide the raw materials your body needs to maintain and repair cartilage. Vitamin C is especially important for collagen synthesis.
- Reduce Sugar and Refined Carbohydrates: High-sugar diets promote insulin resistance and chronic inflammation, both of which are directly linked to metabolic osteoarthritis. Replace sugary snacks with whole foods to protect your joints from the inside out.
- Stay Hydrated: Cartilage is about 80% water. Proper hydration keeps joint cartilage lubricated and resilient. Aim for at least eight glasses of water per day, more if you exercise or live in a warm climate.
- See Your Doctor Early for Joint Pain: Do not dismiss persistent joint stiffness, swelling, or pain as normal aging. Early evaluation allows for earlier intervention, and catching cartilage loss before it becomes severe gives you the best chance at preserving joint function long-term.
Source:
Dong, Y., Zhu, H., Chen, L., Huang, Y., Christen, W., Cook, N. R., Copeland, T., Mora, S., Buring, J. E., Lee, I., Costenbader, K. H., & Manson, J. E. (2022). Effects of Vitamin D3 and Marine Omega-3 Fatty Acids Supplementation on Biomarkers of Systemic Inflammation: 4-Year Findings from the VITAL Randomized Trial. Nutrients, 14(24), 5307. https://doi.org/10.3390/nu14245307








 Subscribe to Ask Dr. Nandi YouTube Channel
Subscribe to Ask Dr. Nandi YouTube Channel










