In a world where instant solutions are highly sought after, cortisone injections have emerged as a popular choice for managing hip and knee pain, joint pain, and inflammation. These seemingly convenient shots promise quick relief for those suffering from hip and knee discomfort.
However, as the popularity of cortisone injections soars, so does the concern surrounding their potential risks and long-term effects. Are these injections truly the magic bullet for joint pain, or is there more to the story?
What Is a Cortisone Shot?
A cortisone shot, also known as a “corticosteroid” or “steroid shot,” is a type of injection that contains a synthetic version of the hormone cortisol. It is used to relieve pain and reduce inflammation in joints, muscles, or connective tissues.
Unlike traditional pain relievers, cortisone shots are not meant to provide immediate relief but rather target the underlying inflammation that leads to pain. These shots are commonly used to manage symptoms of various painful inflammatory conditions, such as arthritis, bursitis, tendonitis, sports injuries, back pain, and gout.
How Cortisone Shot Works
Inflammation is the body’s natural defense mechanism to protect against injuries or foreign substances. However, excessive inflammation can lead to pain and discomfort. When inflammation occurs, substances like bradykinin and histamine are released, irritating nerves and transmitting pain signals to the brain.
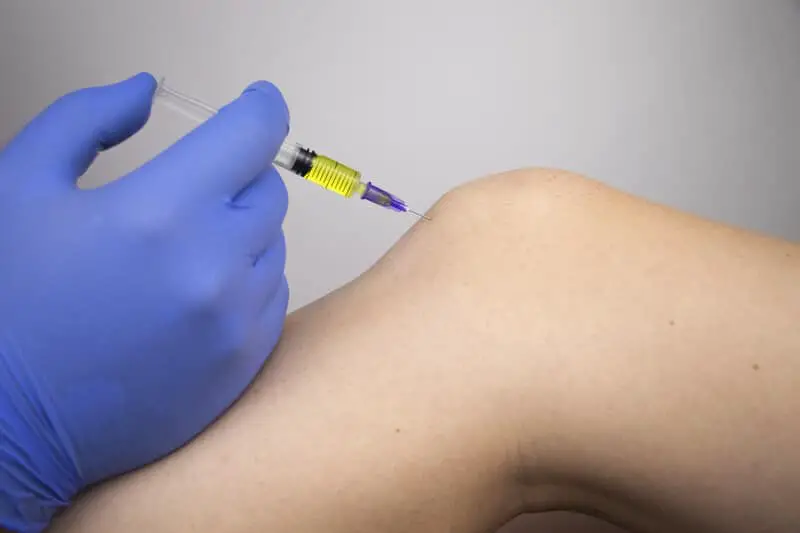
The cortisone shot works by delivering cortisone, a type of corticosteroid, into the affected area using a thin needle. Corticosteroids are synthetic drugs that mimic the hormone cortisol, which is naturally produced by the adrenal glands. It plays a vital role in the body, including suppressing the activity of the immune system.
The effects of cortisone shots can be fast-acting, with some individuals experiencing relief within a few hours while others may take a few days. The duration of pain relief can vary, ranging from weeks to several months, depending on factors such as the treated body part, the dosage administered, and the individual’s response to the shot.
The Dangers of Cortisone Shots Uncovered: Study
A recent study from Boston University unveiled crucial insights into the potential dangers of cortisone injections. The study focused on 459 patients who had received cortisone injections in the knee or hip in a US hospital in 2018.
What the researchers found was alarming. Among those who underwent follow-up radiography or MRI, 36 patients (8% of the cortisone injection recipients) experienced adverse events in their joints. These negative joint effects included problems like faster osteoarthritis progression, subchondral insufficiency fracture, complications of osteonecrosis, and rapid joint destruction with bone loss. [1,2]
It’s important to remember that these risks might extend beyond what the study initially observed. Another 2019 study by a team at Massachusetts General Hospital focused on cortisone injections in the hip. They discovered that patients who received cortisone shots in the hip were more likely to face osteoarthritis progression three to 12 months after the injection. [3]
These findings emphasize that while cortisone injections can provide relief for some, they come with potential risks that must be considered carefully. Talking to healthcare professionals is vital to make informed decisions about the best approach for managing joint pain and inflammation.

Risks and Side Effects of Cortisone Injections
Cortisone injections can offer quick relief for joint pain and inflammation, but it’s essential to be aware of the potential risks and side effects associated with their use. Studies have indicated that the likelihood of side effects increases with larger doses and repeated injections. Among the risks and side effects are:
- Joint tissue damage and deterioration, including cartilage damage and thinning of nearby bone.
- Increased risk of infections, which can be particularly concerning for individuals with compromised immune systems.
- Cortisone flare, causing a temporary increase in pain and inflammation at the injection site
- Impact on blood sugar levels in diabetic patients, potentially leading to complications in managing diabetes
- Long-term side effects with higher doses and frequent shots, including thinning of the skin, easy bruising, weight gain, facial puffiness, and elevated blood pressure
- Possible contribution to cataract formation and osteoporosis with long-term cortisone use
- Rare but severe condition of avascular necrosis, causing damage to the bones of large joints
Expert Recommendations for Safer Cortisone Injection Use
The study authors emphasize the importance of thorough patient education. They recommend that doctors discuss the full spectrum of potential side effects with patients when weighing treatment options. This enables patients to make informed choices regarding their care and the potential risks involved.
For patients who may not have osteoarthritis or have only a mild form of it, experts urge caution when considering cortisone injections. These shots could lead to the development of progressive joint space loss or osteoarthritis. Such patients should also be informed about alternative treatment options available to them.
Additionally, the researchers propose a proactive approach to monitoring joint health. Doctors are advised to order imaging of the joints both before initiating cortisone injections and during follow-up visits. This practice allows medical professionals to track joint and bone changes over time, intervening before the condition worsens and ensuring early management and intervention. [1,2]

My Personal RX for Inflammatory Pain
Dealing with inflammation and the discomfort it brings, particularly in the knees and hips, can significantly impact one’s daily life. When seeking relief from joint pain, it’s essential to be aware of the potential risks of cortisone injections. While medical interventions are crucial, a holistic approach that encompasses lifestyle changes and natural remedies can offer additional relief and support.
- Mindful Movement: Engage in gentle exercises like tai chi or gentle yoga that emphasize fluid movement and flexibility. These practices not only soothe joint pain but also promote relaxation, easing both physical discomfort and mental stress.
- Hydration and Nutrition: Stay hydrated and choose foods rich in omega-3 fatty acids, such as walnuts and flaxseeds, which have anti-inflammatory benefits. Hydration supports joint lubrication and overall cellular health.
- Holistic Wellness: Explore my free Protocol for Optimizing Your Health and Wellbeing, a comprehensive guide to transformative health practices. This resource offers insights into holistic pain management strategies and empowers you to take charge of your well-being.
- Herbal Allies: Incorporate herbs with anti-inflammatory properties into your diet. Turmeric, ginger, and green tea are known for their natural inflammation-fighting abilities and can be consumed in teas and smoothies or as seasonings.
- Turmeric Power: Integrate the Complete Turmeric Matrix into your daily routine. This natural supplement harnesses the potency of turmeric, offering a holistic approach to reducing inflammation and promoting joint health.
As always, it is essential to discuss your specific health situation with a healthcare professional to determine the best course of action and make informed decisions regarding your treatment plan.
Sources:
- Kompel, A. J., Roemer, F. W., Murakami, A. M., Diaz, L. E. P., Crema, M., & Guermazi, A. (2019c). Intra-articular corticosteroid injections in the hip and knee: perhaps not as safe as we thought? Radiology, 293(3), 656–663. https://doi.org/10.1148/radiol.2019190341
- Prior, R. (2019, October 18). Steroid injections may lead to more long-term harm than previously thought, new study says. CNN. https://edition.cnn.com/2019/10/17/health/steroid-injections-study-trnd/index.html
- Simeone, F. A., Vicentini, J. R. T., Bredella, M. A., & Chang, C. Y. (2019). Are patients more likely to have hip osteoarthritis progression and femoral head collapse after hip steroid/anesthetic injections? A retrospective observational study. Skeletal Radiology, 48(9), 1417–1426. https://doi.org/10.1007/s00256-019-03189-x











 Subscribe to Ask Dr. Nandi YouTube Channel
Subscribe to Ask Dr. Nandi YouTube Channel










