Inflammatory Bowel Disease (IBD) affects approximately 1.6 million people across the United States, with up to 70,000 new cases diagnosed each year. (1) If you or someone you love is suffering from this condition, you know it can significantly diminish one’s quality of life. Because I have worked with hundreds of patients with IBD, I am passionate about supporting IBD research and improving my patients’ lives as much as possible.
In this post, I want to discuss Inflammatory Bowel Disease in depth so you can better understand the disease, how it affects the body, what you can do to treat it, and how to best work with your doctor to find healing and support.
What Is Inflammatory Bowel Disease (IBD)?
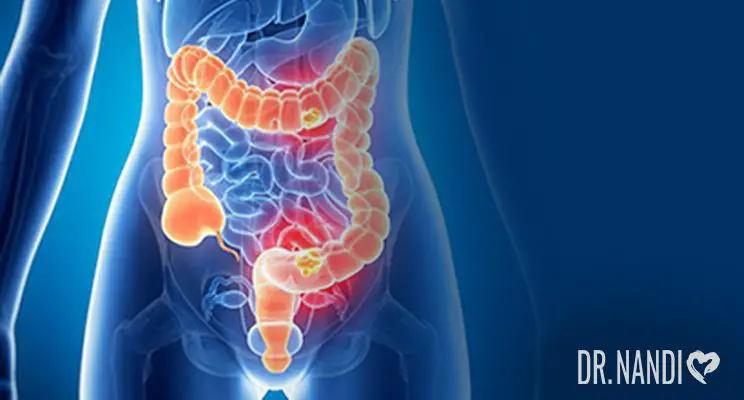
There are two types of inflammatory bowel disease: Ulcerative Colitis and Crohn’s disease; both are chronic inflammatory conditions of the gastrointestinal (GI) tract and may occur together or separately. Today, these are chronic conditions that do not have a cure. Many treatment options can improve or even eliminate some symptoms but not entirely rid one of the disease.
Ulcerative Colitis
Ulcerative Colitis occurs only in the large intestine and the rectum. It happens when chronic inflammation causes damage to the first inner layer of the colon or rectum lining.
Crohn’s Disease
Crohn’s disease can happen anywhere in the GI tract (from mouth to rectum). It occurs when chronic inflammation damages multiple layers of the lining of the GI tract. Crohn’s disease generally begins in the small intestine and spreads to other areas.
Symptoms of IBD
- Persistent diarrhea
- Constipation
- Urgent need to go to the bathroom
- Abdominal pain
- Unexplained Weight Loss
- Small appetite
- Chronic fatigue
Symptoms Unique to Crohn’s Disease
- Mouth sores between gums and lower lip, or bottom of the tongue
- Anal tears, ulcers, infections, or narrowing
Symptoms More Common With Ulcerative Colitis
- Rectal bleeding
- Anemia
Complications of Ulcerative Colitis
When IBD goes untreated for long enough, it can lead to some painful complications that require urgent medical attention. Here are some of the most common complications associated with ulcerative colitis:
- Anemia. It is a condition where your blood doesn’t have enough healthy red blood cells to carry oxygen throughout your body. Anemia can make you feel tired and weak.
- Bleeding. IBD can cause ulcers in the colon, leading to heavy bleeding that may require blood transfusions.
- Toxic megacolon. It is a severe but rare complication characterized by an enlarged and distended colon that becomes filled with gas and fluids. This condition requires immediate medical attention to prevent rupturing of the colon walls.
- Fistulas. Fistulas are abnormal tunnels that form between different organs or between the skin and an organ. They can cause severe pain and may require surgery to repair.
- Kidney stones. People with IBD are more likely to develop kidney stones due to a build-up of waste products in the urine.
- Osteoporosis. This condition is characterized by low bone mass and density, leading to fragile bones that are more likely to break. Osteoporosis is prevalent among IBD people who take corticosteroids to manage their symptoms.
Complications of Crohn’s Disease
- Malabsorption/Malnutrition. Damage to the intestinal tract makes it difficult to digest and absorb nutrients properly.
- Fistula. Ulcers on the intestinal wall develop and create a tunnel to other parts of the intestine or even other organs.
- Stricture. Intestinal narrowing/blockage due to scaring.
- Abscess. Painful collection of pus located somewhere on the digestive tract, often at infection sites.
- Blood Clots. Deep vein thrombosis or pulmonary embolism. IBD patients have a three times greater risk of experiencing blood clots than those without IBD. (13)
- Colorectal Cancer. Those with Crohn’s Disease are more likely to develop colorectal cancer, and the risk increases the longer one has had the disease. Statistics say as many as 18% of people who have had Crohn’s Disease for 30+ years will have developed colorectal cancer. (12)
Other IBD Symptoms Outside The GI Tract
- Red, painful, itchy eyes
- Sores in the mouth
- Swollen, painful joints
- Ulcerations, sores, or rashes on the skin
- Osteoporosis
- Kidney stones
- Liver problems (rare)
IBD vs. IBS
IBD and IBS (Irritable Bowel Syndrome) are different conditions and should not be confused. Although some symptoms may be similar (diarrhea, constipation, abdominal cramps), IBS does not cause severe damage to the GI tract as does IBD. IBS is much less painful than IBD and can often be improved with simple lifestyle changes.
Who Is At Risk For IBD?
The exact cause of IBD is currently unknown, although many factors seem to contribute to its development. These include a genetic disposition for IBD, a poorly functioning immune system, and/or specific environmental triggers.
Genetics
Studies have found that 5-20% of people who develop IBD have a close relative who also has the disease. (2) This means children of parents with IBD have a higher risk than those with parents who don’t have IBD. (3) Research has also found that children have a 36% chance of developing the disease if both parents have IBD. (4)
Certain genetic mutations have been linked to IBD, although having them does not mean you will develop IBD. For example, a particular genetic mutation, the NOD2/CARD15 gene, exists in approximately 20% of Crohn’s Disease patients. (5)
Environmental Triggers
Some environmental/lifestyle triggers have been linked to an increased risk for IBD.
Smoking
People who smoke tobacco regularly are twice as likely to develop Crohn’s Disease as those who do not smoke. (6)
Heavy Antibiotic Use
Some studies suggest that mothers who frequently use antibiotics, which results in changes to the microbiome in the gut, may cause an increased risk of IBD in their children. When a mother gives birth, her microbiome is passed in part to her baby. If her microbiome is weak or imbalanced, it may lead to an increased risk of health issues in the baby later on. (7)
Frequent Nonsteroidal Anti-inflammatory Drug Use
Examples are taking ibuprofen or naproxen. Research has found that frequent NSAIDs may irritate the gut and increase the risk for Crohn’s Disease and Ulcerative Colitis. (8)
Appendectomy
Some studies have found that the risk for developing IBD increases in individuals who have had their appendix removed. The risk is highest in the first six months after removal and slowly declines over the next 20 years. Women have a slightly higher risk than men. (9, 10)
Poor Diet
Food alone does not cause IBD, but certain foods can aggravate it. These include:
- Fatty, fried foods
- Spicy foods
- Meats
- High-fiber fruits and vegetables
- Caffeine
- Sweets, high sugar beverages, and snacks
- Alcohol
Am I At Risk?
Here are some statistics for different demographics:
- Location: More cases of IBD are found in developed countries than in non-developed. There are more people with IBD in urban areas. Northern climates have higher rates than southern. Another interesting statistic; people who immigrate to America from underdeveloped nations have a higher chance of developing IBD.
- Age: People are more likely to be diagnosed with IBD between 15 and 35.
- Gender: Men and women are equally at risk for ulcerative colitis and Crohn’s disease.
- Race: IBD does not seem to affect any race or ethnicity more than another.
How Is IBD Diagnosed?
Although science has yet to find a cure for IBD, there are many treatment options to alleviate symptoms and improve the overall quality of life. There is no one-size-fits-all regimen, and doctors approach treatment case-by-case. The first step is obtaining a proper diagnosis.
Step One: Patient History and Physical Exam
When you initially go to the doctor’s office, you will give your complete health history and tell the doctor about your symptoms. If you want help with this first doctor’s visit, use our Inflammatory Bowel Disease Doctor’s Checklist. It will help you remember all your symptoms and questions so that your visit can be as productive as possible.t
You will also want to discuss your family history. Does anyone in your family have Crohn’s Disease or Ulcerative Colitis?
Your doctor may also perform a basic exam, including a rectal exam.
Step Two: Diagnostic Testing
The following are the most common diagnostic procedures for IBD: (11)
- Blood tests. Your blood will be drawn from an arm vein or a finger prick. Blood testing alone cannot diagnose IBD but can indicate inflammation levels in the body. Chronic inflammation is a marker for IBD. Blood tests can also determine liver and kidney function, detect anemia and check for infection.
- Stool samples. Proteins found in your stool can help to detect inflammation in the body. Other biomarkers in the stool may be used to detect IBD activity. A stool sample can also help to rule out other gastrointestinal conditions that may present similar symptoms as IBD.
- Endoscopy. A tiny camera is used to see inside your body during this procedure. It allows the doctor to see the inside of your intestine and check for damage and signs of IBD.
- Biopsy. Many doctors will also take biopsy samples of your intestinal lining to evaluate inflammation and infection during an endoscopic procedure.
- Colonoscopy. It is the most common type of endoscopy used to diagnose IBD, as the colon tends to be a significant place for symptoms. There are a few steps to having this done:
- You will receive restrictive diet instructions.
- You will be asked to drink a “bowel preparation” drink which will help to eliminate any fecal matter from your digestive tract that would otherwise block the endoscope.
- You will be sedated for the procedure to minimize discomfort.
- A trained professional will insert the colonoscope through your rectum and entire colon.
- Radiology Scans. Two-thirds of the small intestine is not visible using a colonoscopy or endoscopy. These will be viewed using diagnostic imaging like CT scans, MRIs, ultrasounds, and x-rays.
Conventional Treatments for IBD
There are five different medications used to treat IBD and surgery for more complicated cases. Your doctor will most effectively create a plan that fits your unique situation and symptoms.
The five types of medication used to treat IBD are:
- Aminosalicylates. These drugs help to decrease inflammation in the digestive tract. Sulfasalazine (Azulfidine) is an aminosalicylate.
- Corticosteroids. These drugs also help to decrease inflammation. Prednisone is a common corticosteroid used to treat IBD.
- Immunomodulators. These drugs help decrease immune system activation, leading to inflammation in the digestive tract.
- Antibiotics. Sometimes antibiotics are prescribed with other medications, especially during flare-ups or if an infection is present.
- Biologic agents. These are newer drugs that help to target specific proteins involved in the inflammatory response. Infliximab (Remicade) is an example of a biological agent used to treat IBD.
Approximately 33% of people with Ulcerative Colitis will require surgery after 30 years with the disease. About 70% of people with Crohn’s Disease end up needing surgery at one point or another.
Lifestyle Treatments for IBD
These lifestyle changes can help you to manage your IBD symptoms. Because every case is different, work with a medical professional to personalize these to your needs.
Stop Smoking
Those who smoke tobacco regularly are twice as likely to develop Crohn’s Disease as those who do not smoke. (6)
Eat Smaller, More Frequent Meals
Eating smaller meals tends to be easier on digestion in people with IBD. So instead of large meals 2-3 times a day, eat 4-6 small meals throughout the day.
Eat The Right Kind Of Fiber
People with IBD generally have a difficult time digesting high amounts of fiber. However, fiber is still important in one’s diet. Try sticking to soluble fibers like oatmeal, flax-seed, beans, berries, apples, oranges, dried peas, cucumber, carrots, and celery. Avoid insoluble fibers.
Start Walking
Exercise can be a challenge for those with IBD, often because of painful symptoms or the need to be near a bathroom. But many patients with IBD report improvement in symptoms when they walk a little every day. Exercise benefits the whole body, including the digestive system. Start with just a few minutes a day and slowly build up.
Avoid Trigger Foods
Pay close attention to your diet and how each meal affects your symptoms. Avoid foods that aggravate your IBD. These may include:
- dairy
- chocolate
- cruciferous vegetables
- wheat
- broccoli
- beans
- alcohol
- tap water
- emulsifiers
- fatty foods
- caffeine
If you are not sure what foods make your symptoms worse or everything you eat makes them worse, your doctor may recommend a temporary liquid diet. It gives your digestive system a chance to rest and heal. After a short period, you will begin to reintroduce regular food; slowly, pay attention to how each piece affects your system.
Only do a liquid diet under the direction of your physician.
Find Support
Connecting with people who understand what you are going through can be tremendously helpful. Look for support groups on social media as well as in your community.
Test for Nutritional Deficiencies
Ask your doctor to perform a test for nutritional deficiencies. It makes it easy to see what you are not absorbing well so you can supplement as needed. Use vitamins and minerals from brands recommended by your doctor, as the supplement market is not carefully regulated. You may also want to work with a dietitian to fine-tune your diet.
Use Turmeric and Probiotics
Curcumin, the active ingredient in turmeric, has been studied extensively for its anti-inflammatory properties. Research has found that it may be beneficial for those with IBD. (13) I also recommend my patients try a high-quality probiotic. Though the benefits have not been proven for IBD specifically, I find many people experience better digestion/absorption when they take them daily.
Heading to the Doctor? Here is a Doctor Checklist for IBD.
Frequently Asked Questions
Can inflammatory bowel disease kill you?
A. Crohn’s Disease and Ulcerative Colitis are not considered fatal conditions. There are rare cases where patients have died from IBD-related causes.
Can inflammatory bowel disease cause cancer?
A. People with IBD are more likely to develop colorectal cancer than those without IBD. This risk increases the longer one has had the disease.
Can inflammatory bowel disease be cured?
A. At this time, there is no cure for inflammatory bowel disease. However, many medications and treatments can reduce symptoms and improve quality of life.
What is idiopathic inflammatory bowel disease?
A. When IBD has an unknown cause.
Conclusion
If you think you might have IBD, I suggest scheduling an appointment with your healthcare professional. Here is a Doctor Visit Checklist to help you have the most productive visit possible.
I believe strongly that we all should be our own #HealthHero. It means that we are committed to our well-being and will do what it takes to live a life of health and vitality. When you feel your best, you can make the most impact in the lives of those you love and in the community you live in.
Did you find the information in the post helpful? What other conditions would you be interested in learning about on our blog? Comment below.
References
- http://www.crohnscolitisfoundation.org/assets/pdfs/updatedibdfactbook.pdf
- Russell RK, Satsangi J. Does IBD run in families? Inflamm Bowel
Dis. 2008;14(S2):S20-S21 - Ephgrave K. Extraintestinal manifestations of Crohn’s disease.
Surg Clin North Am. 2007;87(3):673-680 - Bennett RA, Rubin PH, Present DH. Frequency of inflammatory
bowel disease in offspring of couples both presenting with
inflammatory bowel disease. Gastroenterology.
1991;100:1638-1643. - Noomen CG, Hommes DW, Fidder HH. Update on genetics
in inflammatory disease. Best Pract Res Clin Gastroenterol.
2009;23(2):233-243. - Cosnes J. What is the link between the use of tobacco and IBD?
Inflamm Bowel Dis. 2008;14 (Suppl 2):S14-S5 - https://nyulangone.org/press-releases/changes-in-bacterial-mix-linked-to-antibiotics-increase-risk-for-inflammatory-bowel-disease
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3369539/
- https://www.ncbi.nlm.nih.gov/pubmed/9247453
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2000241/
- http://www.crohnscolitisfoundation.org/assets/pdfs/diagnosing-and-managing-ibd.pdf
- Eaden JA, Abrams KR, Mayberry JF. The risk of colorectal cancer
in ulcerative colitis: a meta-analysis. Gut. 2001;48(4):526-535. - Nguyen GC, Sam J. Rising prevalence of venous thromboembolism
and its impact on mortality among hospitalized inflammatory
bowel disease patients. Am J Gastroenterol.
2008;103(9):2272-2280 - https://www.ncbi.nlm.nih.gov/pubmed/21649456








 Subscribe to Ask Dr. Nandi YouTube Channel
Subscribe to Ask Dr. Nandi YouTube Channel










