You have probably seen measles making headlines again. Outbreaks are popping up in communities across the world, filling emergency rooms and alarming public health officials. But what makes measles so difficult to contain? The answer lies in a single number that puts this virus in a league of its own. Measles is not just contagious. It is one of the most transmissible infectious diseases ever documented, capable of spreading through the air and lingering in a room long after an infected person has left. Understanding how it moves, how it compares to other viruses, and why vaccination coverage matters more for measles than almost any other disease is essential for anyone trying to protect themselves and their families.
The Number That Tells You Everything: R0
Scientists measure how contagious a disease is using a value called the reproduction number, or R0 (pronounced “R naught”). R0 represents the average number of new infections one sick person will cause in a population where nobody is immune.
If R0 is less than 1, the disease will eventually die out because each case produces fewer than one new infection. If R0 is greater than 1, the disease will spread. The higher the number, the faster and more explosively it spreads.
Demographer Alfred Lotka first proposed the reproduction number in the 1920s. By the 1950s, epidemiologist George MacDonald applied it to malaria and established the principle that public health interventions should aim to push R0 below 1.
During the early days of the COVID-19 pandemic, R0 became a household term. Scientists estimated SARS-CoV-2 had an R0 somewhere between 1.5 and 3.5. That was enough to cause a global pandemic that shut down economies and overwhelmed hospitals worldwide. Now consider measles: its R0 ranges from 12 to 18.

Measles Makes Other Viruses Look Slow
To appreciate what an R0 of 12 to 18 means, compare it to some of the most feared diseases in history. Smallpox, one of the deadliest diseases humanity has ever faced and the only human disease successfully eradicated, had an R0 of 5 to 7. Polio sits in a similar range. The Ebola virus that caused the devastating 2014 West Africa outbreak had an R0 of roughly 1.5 to 2.5. Seasonal influenza comes in at 0.9 to 2.1.
Against all of those, measles towers above at 12 to 18. In practical terms, that means one person with measles in an unprotected population could infect 12 to 18 others. Each of those 18 could infect 18 more. Within just a few transmission cycles, a single case can explode into hundreds.
An important caveat: R0 measures only how infectious a disease is, not how severe or deadly it is. Ebola kills a far higher percentage of the people it infects than measles does. But in terms of pure transmissibility, measles operates on a different scale than almost any other pathogen.
How Measles Actually Spreads
Raw numbers alone do not explain why measles is so hard to contain. The way it travels matters just as much.
Measles is airborne. When an infected person breathes, coughs, or sneezes, they release tiny droplets containing the virus into the surrounding air. Those droplets can remain infectious in a room for up to two hours after the person has left.
You do not need to be standing next to someone with measles to catch it. You do not even need to be in the same room at the same time. If an infected person was in a waiting room, grocery store, or airport terminal, and you walk in afterward, you can still contract the virus from the air and surfaces they left behind.
That is why public health departments issue exposure alerts for specific locations during outbreaks. A single case at a busy airport can put hundreds of people at risk, even if none of them came face-to-face with the infected person.
Nine out of ten unvaccinated people exposed to measles will catch it. That 90% infection rate among susceptible individuals makes contact tracing and containment extremely difficult once the virus gains a foothold in an under-vaccinated community.
The Sneaky Window When You Are Contagious But Do Not Know It
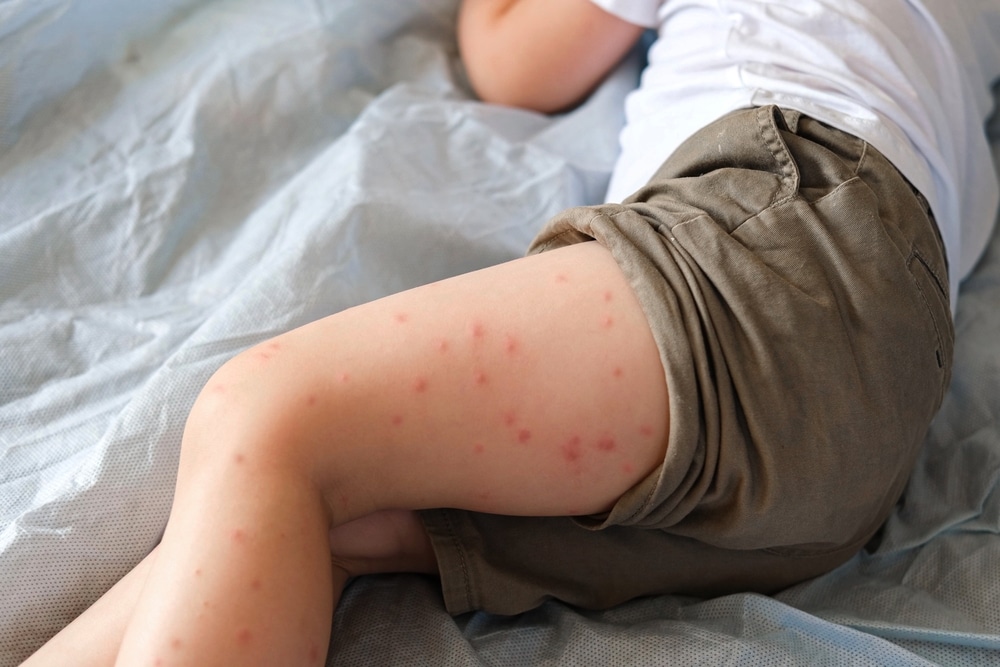
Making matters worse, measles is contagious before you know you have it. An infected person can spread the virus from up to four days before the characteristic rash appears until four days after it shows up.
That creates a window of at least eight days during which someone can infect others. During the early days, before the rash, measles symptoms look a lot like a cold or the flu: fever, cough, runny nose, and watery eyes. Most people would not suspect measles based on those symptoms alone.
By the time the rash appears and measles is recognized, the infected person may have already exposed dozens of people in schools, workplaces, public transit, and other shared spaces. That pre-rash contagious period is one of the main reasons measles outbreaks grow so fast and catch communities off guard.
Why 95 Percent Vaccination Is the Magic Number
Given how contagious measles is, controlling it requires an unusually high level of population immunity. According to the European Centre for Disease Prevention and Control, at least 95% of eligible people must be vaccinated to keep measles at bay.
That threshold exists because of how R0 and herd immunity interact. With an R0 of 12 to 18, the virus can still find enough susceptible people to sustain transmission unless nearly everyone is protected. Even a small dip below 95% coverage opens pathways for the virus to spread.
By comparison, diseases with lower R0 values require lower vaccination thresholds for herd immunity. Polio needs roughly 80% to 85% coverage. Influenza needs even less. But measles demands near-universal vaccination because of its extraordinary transmissibility.
When coverage drops even a few percentage points, outbreaks follow. Data from recent outbreaks around the world consistently show the same pattern: the overwhelming majority of people falling sick are unvaccinated.
The Vaccine That Changed Everything
The development of the measles vaccine was one of the most impactful achievements in medical history. Today’s MMR (measles, mumps, rubella) and MMRV vaccines are both safe and remarkably effective. Two doses provide approximately 97% protection against measles infection.
A 2024 study from the London School of Hygiene and Tropical Medicine confirmed that this protection persists at a strong level for decades. For a virus this contagious, having a vaccine that delivers near-complete, long-lasting immunity is an extraordinary tool.
Before the vaccine became widely available in the 1960s, measles infected an estimated 3 to 4 million people in the United States every year. Hundreds died annually. Thousands were hospitalized with complications, including pneumonia, brain swelling (encephalitis), and permanent hearing loss.
Widespread vaccination drove those numbers down dramatically. By 2000, measles was declared eliminated in the United States, meaning sustained transmission had been stopped. But elimination is not eradication. The virus still circulates globally, and every unvaccinated person represents a potential entry point for it to return.
Who Is Most at Risk
Not everyone can receive the measles vaccine. Babies under 12 months are too young for their first dose. People with certain immune-compromising conditions or medical treatments cannot be vaccinated safely. These groups depend entirely on the people around them being vaccinated, a concept known as herd immunity.
When vaccination rates drop in a community, the people who suffer first and most are those who cannot protect themselves: infants, cancer patients undergoing chemotherapy, organ transplant recipients, and others with weakened immune systems.
Adults who missed childhood vaccines or received only one dose instead of the recommended two may also have incomplete protection. Health authorities worldwide carry a clear message: it is never too late to check your immunization status, catch up on missed doses, or make sure your children are up to date.

Why Outbreaks Keep Happening
If the vaccine is so effective and widely available, why do outbreaks keep returning? The answer lies in pockets of low vaccination coverage, whether due to vaccine hesitancy, access barriers, misinformation, or disruptions to routine immunization programs (as happened during the COVID-19 pandemic when many children missed scheduled vaccinations).
A community needs 95% coverage to stop measles transmission. When any neighborhood, school, or social group falls below that threshold, the virus has an opening. And with an R0 of 12 to 18, it does not need a large opening. A handful of unvaccinated individuals in the same social network is enough to spark an outbreak that can spread rapidly before public health teams can respond.
The current wave of outbreaks is a direct reminder that measles has not gone away. It is still circulating globally, still extraordinarily contagious, and still ready to exploit any gap in protection. Vaccination remains the most powerful, most proven tool available to keep it under control.
My Personal RX on Protecting Your Family Against Measles and Boosting Immune Health
Measles is one of the most contagious diseases in the world, and vaccination is by far the most effective protection. But immune health goes beyond any single vaccine. A strong, well-nourished immune system responds better to vaccines, fights infections more effectively, and recovers faster when illness strikes. I tell my patients that immune defense starts with daily habits. Here is what I recommend:
- Get Vaccinated and Stay Up to Date: If you or your children have not received two doses of the MMR vaccine, schedule them now. Two doses provide 97% protection. Check your immunization records and catch up on any missed doses, regardless of your age.
- Prioritize Deep Sleep Every Night: Your immune system produces infection-fighting cytokines and T cells during deep sleep. Sleep Max combines magnesium, GABA, 5-HTP, and taurine to promote restorative REM sleep so your body can build and maintain strong immune defenses.
- Fill Your Nutrient Gaps After 40: Declining nutrient absorption weakens immune function with age. Download my free guide, The 7 Supplements You Can’t Live Without, to learn which supplements support immunity, which “healthy” foods may be misleading you, and how to identify quality products.
- Wash Hands Frequently During Outbreaks: While measles is airborne, hand hygiene reduces your overall exposure to respiratory pathogens. Wash with soap and water for at least 20 seconds, especially after being in public spaces.
- Exercise for 30 Minutes Daily: Moderate physical activity improves immune cell circulation and reduces chronic inflammation. Walking, cycling, and swimming all strengthen your body’s ability to detect and respond to infections.
- Manage Stress to Protect Immune Function: Chronic stress suppresses both innate and adaptive immunity. Practice daily breathwork, meditation, or time outdoors to keep cortisol levels in check and your immune system responsive.
- Keep Your Children’s Vaccines on Schedule: Missed or delayed childhood vaccines leave children vulnerable during peak exposure years. Work with your pediatrician to ensure all recommended immunizations are completed on time.
- See a Doctor Immediately If You Suspect Measles Exposure: If you or your child develops fever, cough, runny nose, and a rash after potential exposure, contact your healthcare provider before visiting a clinic. Early notification helps prevent further spread in waiting rooms and healthcare settings.
Source: Tahir, I. M., Kumar, V., Faisal, H., Gill, A., Kumari, V., Tahir, H. M., & Haque, M. A. (2024). Contagion comeback: unravelling the measles outbreak across the USA. Frontiers in Public Health, 12, 1491927. https://doi.org/10.3389/fpubh.2024.1491927









 Subscribe to Ask Dr. Nandi YouTube Channel
Subscribe to Ask Dr. Nandi YouTube Channel










